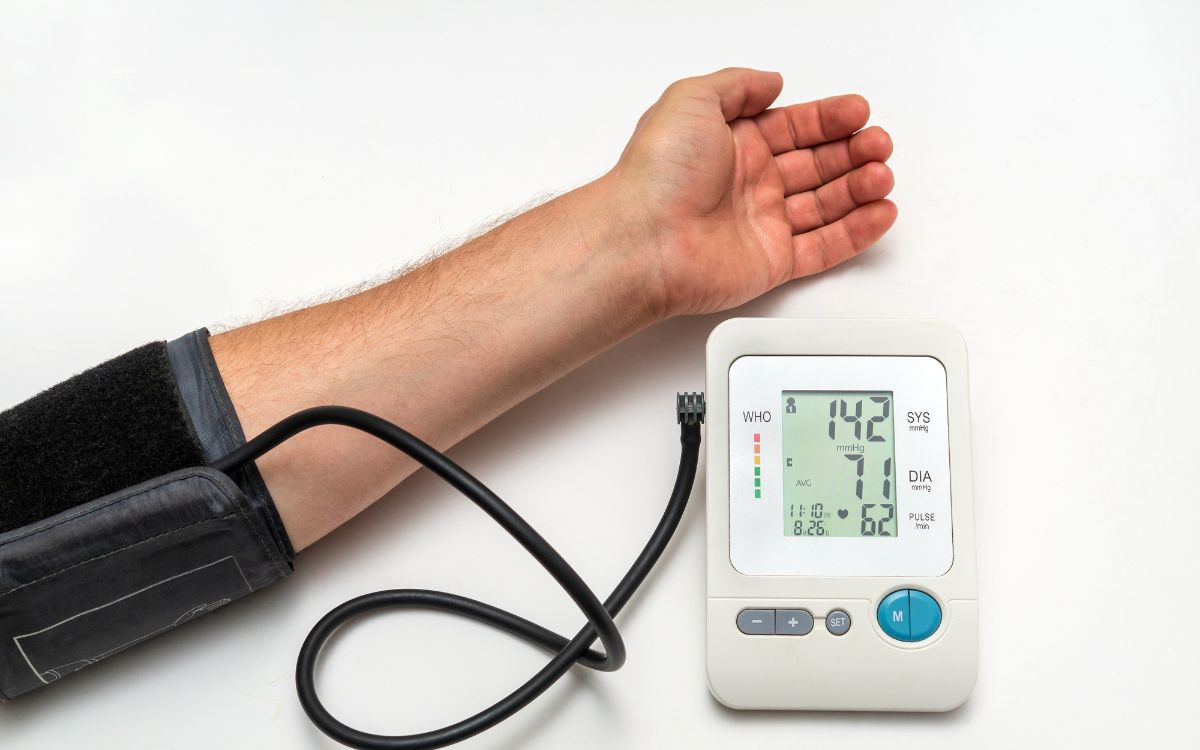
Blood pressure. Two numbers. Simple, right? Not always. Especially at home. Especially for older adults. High blood pressure is a silent threat. It damages hearts, brains, kidneys. Knowing your numbers is crucial. Home monitoring gives valuable information. It helps doctors. It helps you.
But… mistakes happen. Small errors lead to big misreadings. False highs. False lows. Wrong readings mean wrong decisions. Medication changes that aren’t needed. Or dangerous delays in treatment. For seniors, getting it right is extra important. Bodies change with age. Blood vessels stiffen. Pressure can swing more easily.
Let’s talk about the common home blood pressure monitoring mistakes elderly patients often make. And how to fix them. Get your readings right. Take control.
Mistake #1: The Wrong Cuff Size (This is HUGE!)
This is the biggest error. Maybe the most common. The cuff must fit your arm correctly. Too small? Your readings will be falsely high. Too big? Readings may be falsely low. Both are bad.
The Problem: Arms change. Muscle mass decreases. Fat distribution shifts. The cuff that fit ten years ago might not fit now. Many people use the cuff that came with the machine. They never check if it’s right.
The Fix: Measure your upper arm. Before you buy a monitor. Or if you already have one. Use a simple tape measure. Measure around the bare middle of your upper arm. Midway between shoulder and elbow. Do this yourself or get help.
-
Standard Adult Cuff: Fits arm circumferences of 22-32 cm (about 8.5 – 12.5 inches). Most common size.
-
Large Adult Cuff: Needed for arms 32-42 cm (12.5 – 16.5 inches). Crucial if your arm is bigger.
-
Small Adult Cuff: For arms 17-22 cm (6.5 – 8.5 inches). Often needed for very slender arms.
Check the box. Your monitor’s cuff will list its range. Does your arm measurement fit? If not, you need a different cuff. Tell your doctor your arm size. They can help. Never guess.
Mistake #2: Bad Timing, Bad Routine
Taking your pressure whenever you feel like it? Right after coffee? Right after arguing with the neighbor? Right after rushing to answer the phone? Bad idea. Inconsistent timing wrecks useful data.
The Problem: Blood pressure changes constantly. It dips and rises naturally. Stress, activity, caffeine, nicotine, meals – all affect it. Taking readings randomly gives a messy picture. It doesn’t show your true baseline. Doctors need patterns.
The Fix: Establish a routine. Consistency is key.
-
Same Times Daily: Most guidelines recommend twice daily. Once in the morning. Once in the evening. Before breakfast and before dinner are good. Before taking any morning blood pressure meds. And before evening meds or bedtime. Pick your times. Stick to them.
-
Wait After Activities: Sit quietly for 5 minutes before measuring. No talking. No TV. No phone scrolling. Just relax. Breathe.
-
Avoid Triggers: Don’t measure within 30 minutes of:
-
Caffeine (coffee, tea, cola)
-
Smoking or vaping
-
A big meal
-
Strenuous exercise
-
A stressful event
-
Mistake #3: Poor Body Position
How you sit matters. A lot. Slouching? Legs crossed? Arm dangling? Feet not flat? All these can change your reading. Often by 10 mmHg or more. That’s significant.
The Problem: Incorrect posture adds strain or changes blood flow. Your body isn’t relaxed. The machine measures extra pressure or not enough pressure. It’s not measuring your true resting pressure.
The Fix: Sit Properly. Every Time.
-
Chair: Use a straight-backed chair. Ditch the sofa or recliner for this moment.
-
Feet: Flat on the floor. No crossing ankles or legs.
-
Back: Sit back comfortably. Support your back.
-
Arm: Rest your arm on a table or desk. The cuff should be level with your heart. Right at mid-chest height. Your arm should be fully supported. Relaxed. Palm up.
-
Cuff: Place it directly on bare skin. Not over clothing. The bottom edge should be about 1 inch (2-3 cm) above your elbow bend. The tube should run down the center of your inner arm.
Mistake #4: Talking or Moving During the Reading
The machine inflates. It feels tight. You talk to your spouse about dinner. Or you wiggle your fingers. Or you shift in your seat. Mistake.
The Problem: Any movement or talking engages muscles. It can briefly increase blood pressure. The machine is sensitive. It picks up these changes. Your reading goes up. It’s not your resting pressure.
The Fix: Be Still. Be Silent. Breathe Normally.
-
Sit quietly throughout the entire measurement.
-
Do not talk.
-
Do not move the arm with the cuff.
-
Keep your other hand still too.
-
Focus on breathing slowly and naturally. Don’t hold your breath.
-
Wait until the machine fully deflates and shows the numbers before moving or speaking.
Mistake #5: Not Emptying Your Bladder First
It sounds minor. It isn’t. A full bladder is surprisingly powerful.
The Problem: A full bladder creates physical pressure. It can also cause low-level stress or discomfort. This can easily raise your systolic pressure (the top number) by 10-15 mmHg. That’s enough to misclassify your hypertension stage.
The Fix: Go Before You Go. Make a quick bathroom stop part of your 5-minute pre-measurement quiet time. Every time. Especially before your morning reading.
Mistake #6: Ignoring Machine Maintenance and Calibration
Home monitors are machines. They need care. They aren’t perfect forever.
The Problem: Batteries get weak. Tubes can kink or leak. Cuffs wear out. Machines can drift out of calibration over time. You might get consistently wrong readings and never know. Trusting a faulty machine is dangerous.
The Fix: Treat Your Monitor Well.
-
Check Batteries: Replace them regularly. Or use the AC adapter if available. Low power affects performance.
-
Inspect the Cuff and Tube: Look for cracks, leaks, or stiffness. Ensure the Velcro holds well.
-
Store Properly: Keep it in a clean, dry place. Avoid extreme heat or cold. Don’t leave it in a hot car.
-
Validate Annually: Take your home monitor to your doctor’s office or pharmacy once a year. Check it against their professional, calibrated device. Take it with the cuff you use. Measure your pressure with both machines back-to-back (after resting!). Are the readings within 5 mmHg? If not, your home monitor may need replacing. Tell your doctor about the comparison results.
Mistake #7: Measuring Over Clothing (Especially Thick Sleeves)
Rolling up a thick sweater sleeve? Measuring over a shirt? Convenient? Yes. Accurate? No.
The Problem: Clothing adds bulk. It can interfere with the cuff’s sensors. It prevents the cuff from making proper contact with your skin. Readings become unreliable. Usually falsely high.
The Fix: Bare Skin Contact. Always place the cuff directly on your bare upper arm. Wear a short-sleeved shirt or remove your sleeve completely. A thin t-shirt sleeve underneath is usually okay, but bare skin is best. Avoid bulky sweaters or jackets.
Mistake #8: The “One and Done” Approach
Taking a single reading and calling it a day? Not enough. Especially the first reading.
The Problem: The act of putting on the cuff and starting the machine can cause a slight, temporary rise in pressure for some people. The first reading is often higher than subsequent ones taken immediately after. Relying on just one reading, especially that first one, can give a false high.
The Fix: Take Multiple Readings. Follow this protocol:
-
Sit quietly for 5 minutes (as before).
-
Take your first reading. Note it down.
-
Wait 1-2 minutes. Sit quietly.
-
Take a second reading. Note it down.
-
If the two readings differ by more than 5 mmHg, wait another minute and take a third.
-
Record ALL readings. Take the average of the last two readings. This is the number to record and share with your doctor. Discard the first one if it was much higher.
Mistake #9: Poor Record Keeping (Or None at All)
Relying on memory? Jotting numbers on random scraps of paper? Not writing down the time or date? Useless for your doctor.
The Problem: Doctors need to see trends over time. They need context – time of day, any symptoms. Scattered, incomplete data is hard to interpret. It doesn’t show if your medication is working.
The Fix: Log It Properly. Every time.
-
Date and Time: Always.
-
Systolic (Top Number) and Diastolic (Bottom Number): Clearly.
-
Heart Rate (Pulse): If your monitor shows it.
-
Notes: Any relevant details? Felt dizzy? Just took medication? Had caffeine earlier than planned? Stressed?
-
Use a Log Book or App: Simple notebook dedicated to BP. Or use a blood pressure tracking app on your phone or tablet. Many monitors come with apps that sync via Bluetooth – very convenient. Bring your log (or phone) to every doctor’s appointment.
Mistake #10: Obsessive Monitoring (Checking Constantly)
Feeling anxious? Taking your pressure 10 times a day? Every time you feel slightly off? This creates stress. Stress raises blood pressure. It’s a vicious cycle.
The Problem: Anxiety directly impacts blood pressure. Constant checking fuels the anxiety. You might see normal fluctuations and panic. This leads to unnecessary stress. It doesn’t help manage your condition.
The Fix: Stick to the Schedule. Trust your routine. Measure twice daily as recommended. At your set times. Following the proper steps. That’s enough data. If you feel unwell between your scheduled times, note your symptoms. But resist the urge to grab the cuff constantly. Talk to your doctor about your anxiety. They can help.
Mistake #11: Not Sharing Readings (Or Only Sharing “Good” Ones)
Hiding high readings? Only showing the doctor the “good” numbers? Or forgetting to bring your log altogether? This defeats the purpose.
The Problem: Your doctor needs the real picture. The highs, the lows, the averages. They need to see patterns to make informed decisions about your care. Withholding information can lead to undertreatment. It’s dangerous.
The Fix: Be Honest and Complete. Share your entire log. Every reading from your monitoring period. Bring it to every appointment. Discuss the patterns you see. Ask questions. This is a partnership for your health.
Mistake #12: Not Understanding Your Target Numbers
“High” is vague. What is your target blood pressure? Do you know? It might differ from your neighbor’s.
The Problem: Blood pressure goals are personalized. They depend on your age, other health conditions (like diabetes or kidney disease), and overall risk. Aiming blindly without knowing your target is confusing. You might worry unnecessarily. Or not worry enough.
The Fix: Ask Your Doctor. “What is my target blood pressure?” Get a clear number. Write it down. Keep it with your log. Understand that home readings might be slightly lower than office readings (that’s common and expected). Knowing your goal helps you track progress effectively.
Why Getting It Right Matters More for Seniors
These mistakes matter for everyone. But they matter more for older adults.
-
Greater Risk: The risks of high blood pressure (stroke, heart attack, kidney failure) increase significantly with age. Accurate monitoring is critical for protection.
-
White Coat Effect: Many seniors experience higher readings in the doctor’s office due to anxiety. Home monitoring provides a truer picture of their usual pressure.
-
Frailty: Blood pressure can drop suddenly in older adults (orthostatic hypotension). Accurate home readings help track this.
-
Multiple Medications: Seniors often take several medications. Accurate home readings are vital for doctors to manage these safely and avoid harmful interactions or over/under-treatment.
-
Physical Challenges: Arthritis, tremors, vision problems, or hearing loss can make using the monitor correctly harder. Extra care is needed to overcome these.
Empowerment, Not Fear
Home blood pressure monitoring is powerful. It puts knowledge in your hands. But like any tool, you need to use it correctly. Avoiding these common mistakes ensures the numbers you see reflect reality. They guide safe and effective treatment.
It takes practice. It takes diligence. But it is worth it. Accurate readings mean better care. Better care means a healthier heart, a sharper brain, and more years of good life.
Talk to your doctor or nurse. Show them your monitor. Show them your technique. Ask for feedback. Get your cuff size checked. Validate your machine. Commit to the routine.
Do it right. Know your true numbers. Take control of your heart health. You’ve got this